For many people who experienced childhood trauma, flashbacks and nightmares can be an unwelcome part of life. They can be especially challenging when they show up unexpectedly, leaving you feeling distressed and thrown off course.
This page offers practical strategies to help you respond in the moment and support yourself over time.
Prioritize your well-being
Reading about trauma responses can bring up strong emotions and physical reactions. Go at your own pace, take breaks as needed, and use the StrongAfter Strength Toolkit as needed. Take care.
Part One: Dealing With Flashbacks
What Is a Flashback?
A flashback is when a past traumatic experience is re-lived in the present, and can feel like it’s happening right now. It might come as a brief flash or fragment of memory, or sometimes as a more detailed replay.
Flashbacks can happen at any time of day or night and can take you completely by surprise. They can happen in the first person—where it feels like you’re right there, seeing and experiencing it through your own eyes—or in the third person, like watching a movie where you’re the main character. Sometimes flashbacks replay events or details you weren’t fully aware of at the time, or that you had long forgotten.
- Visual Memories: image (moving and static), scenes, fragments, in high-definition color or black and white, sometimes distorted and foggy
- Auditory Memories: sounds, voices, footsteps, doors, breathing, music
- Emotional Memories: loneliness, distress, hopelessness, rage, terror, dread, danger, or a complete lack of feelings (numbness)
- Body Memories: physical sensations including pain, nausea, gagging sensation, difficulty swallowing, feeling restricted, difficulty breathing
- Sensory Memories: Smells and tastes
- Combinations of any of the above
A Word About Traumatic Memories

Most everyday memories include several connected elements, such as sensations, images, actions, emotions, and meaning. With traumatic memories, these pieces can appear fragmented and disconnected—some parts may appear to be missing, while others feel especially intense or vivid. This can add to confusion and distress.
When a flashback happens, the past and present can get confused. You might feel out of control or like you’re “going crazy.” Your body may react with fight-flight-freeze, pounding heart, shaking, dizziness, muscle tension, or trouble concentrating.
If any of this sounds familiar, you’re definitely not alone, and you deserve care and support.
What Triggers Flashbacks?
Sometimes what triggered a flashback is obvious (like driving past an old school, or seeing something in the news). Other times, flashbacks are linked to bigger life changes (moving, starting a relationship, a new job) or to a particular emotion like fear or panic.
Flashbacks can be particularly challenging because they often arrive without warning, sometimes as partial memories of events you didn’t fully remember or recognize at the time. This can be really intense.
What Can Help
When you’re in the middle of it, it can help to have some practical skills to fall back on to bring some relief.
- Move to safety if you can. If your surroundings (the place or the people) are making it worse, step away to a quieter or safer place.
- Name what’s happening. Tell yourself: “This is a flashback. It’s a memory. I’m safe right here, right now.”
- Avoid analyzing or sifting through the memory mid-flashback. Focus first on calming and grounding. You can choose later whether to reflect on it.
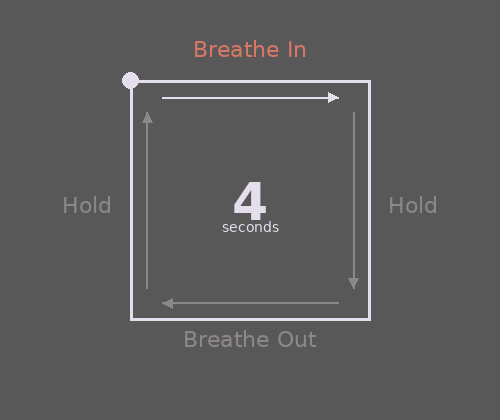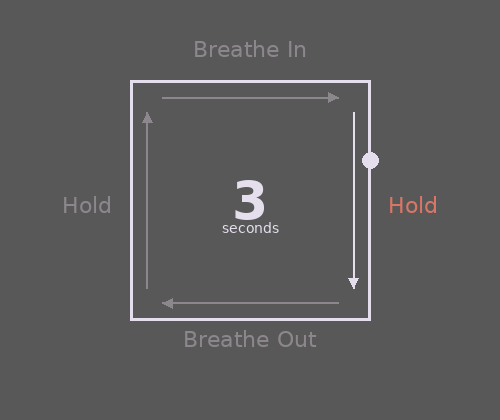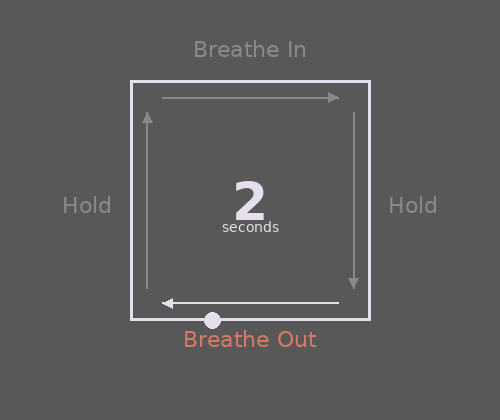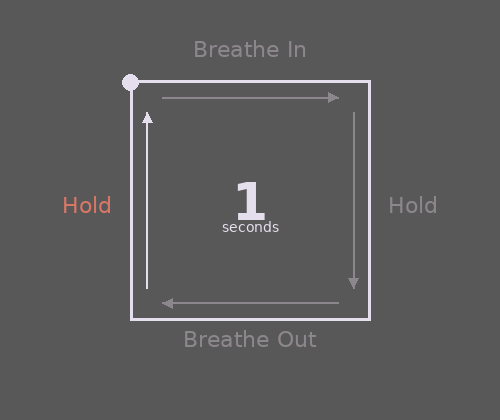
- Breathe slowly and deeply. Often when we’re startled or scared, our breathing becomes fast and shallow, which can reduce oxygen and intensify panic. This can lead to sensations like a pounding head, tightness, shakiness, dizziness, or feeling faint. Try slowing your breath by counting slowly to five as you breathe out—longer exhales help calm your nervous system. A simple option to practice is Box Breathing (try following the gif).
- Practice breathing when you’re not triggered. Deep breathing is a skill that’s easier to use when it’s familiar. Practice when you’re calm, not just when you’re having a flashback or in a stressful situation. Try breathing from your belly, placing a hand just below your navel and letting it rise as you breathe in and fall as you breathe out. Practice regularly.
Distance Yourself From the Flashback by Grounding in the Present
Grounding helps your body and brain re-orient to “now” and distance yourself from the flashback. You can learn more in our StrongAfter Strength Toolkit:

- Check out and practice Grounding Exercises that physically engage you in the present and activate your senses.
- If possible, consciously stretch, move and walk around. Stamp your feet or grind them around on the floor to remind yourself where you are now.
- Make, hold, and take time to taste a drink.
- Hold an ice cube in your hand or place one on the back of your neck.
- Look around, notice what is going in your immediate vicinity: name the people, the place, the furniture, colors etc.
- Listen to the sounds around you: the traffic, voices, the washing machine, etc.
- Actively bring your awareness into the present. The sensations you’re noticing are happening now; the images and memories belong to the past.
Remind Yourself Who You Are Now
Some people find it grounding to say (out loud or silently):
- My name is…
- I am __ years old.
- My address is…
- Today’s date is…
- My job or work is…
- My favorite activity to relax is…
- I can get support or help from…
- What helps me feel grounded and connected to my life is…
Refocus After the Intensity Passes
Once you’re more settled, refocus your mind:

- Think about upcoming tasks, write a to-do list, or record a note on your phone of things to do
- Listen to music, use a calming app on your app, or look at something on your phone that brings good energy into your life (photos, a video, a game)
- Text or call a supportive person
- Ask yourself: “What am I doing next?”
You can also remind yourself: “I can come back to this memory at a time of my choosing.”
That isn’t avoidance; it’s choice and control to decide when, if, and how to review flashbacks.
If Flashbacks Keep Happening

- Make breathing and grounding part of a daily routine so you have them ready when you need them.
- Consider carrying a “present-day anchor” (phone, watch, ring, wristband)—something that clearly belongs to your adult life now and wasn’t part of your past.
- Reach out to a professional (a trauma-informed doctor or therapist) for support.
Connect and Access Support
It can be helpful to let trusted people know you experience flashbacks and what helps, whether that’s helping you slow your breathing, talking to you, getting you a warm drink, or sitting with you. The purpose is to help you reconnect with the present in a safe and supportive way.
Be Kind to Yourself
We’re not underestimating how challenging and overwhelming flashbacks can be. Like a migraine, a flashback can be exhausting and leave you feeling shaken.
In addition, kind, encouraging self-talk is far more helpful than questioning or judging yourself. Check out the Introduction to Self-Compassion in the StrongAfter Strength Toolkit.
Alcohol, Drugs, and Self-Judgment
If you’re cutting back or stopping alcohol or drugs, that can be a positive step. But for some people, reducing “numbing” can lead to a surge of flashbacks or nightmares. If dependence on a substance has been significant, medical support may be required to help the body safely adapt. In addition, this is a time when it is particularly useful to use the StrongAfter Strength Toolkit.
Dealing with flashbacks and nightmares—especially while cutting back on alcohol or drugs—can be made harder by harsh self-judgments about yourself or the change process.
- “I’m too damaged to get through this.”
- “I’m not strong enough.”
- “I’m losing it.”
- “It’s easier not to feel all of this.”
- “This is making everything worse.”
If you notice yourself judging or criticizing yourself, it may be useful to pause and actively shift your focus toward developing Self-Compassion.
Identifying Triggers (With Care)
If flashbacks are interfering with your life, it can help—with appropriate support—to identify what’s triggering them in the present. When a memory is recognized and accepted as something that happened in the past, it often becomes less likely to bother you in the present.

A piece of the puzzle: Although flashbacks are overwhelmingly unwelcome visitors, they can sometimes bring forth information or feelings that help fill in memory gaps. Some men describe how noticing patterns in triggers and flashbacks became a “missing piece” that helped them better understand what happened.
Proceed with care: While becoming aware of triggers can be helpful, it’s important to move cautiously. Any exploration should prioritize safety and focus on identifying present-day triggers rather than revisiting the content of the flashback itself. Focusing too much on the trauma can invite more memories to surface and feel overwhelming.
Consider Professional Support
If you’re experiencing flashbacks, it can help to talk with a qualified trauma-informed therapist or healthcare professional. They can support you with identifying triggers, learning coping skills, and healing in the present—not just revisiting the past.
- How did you become aware of the flashback? What were the signs?
- What was happening when the flashback occurred?
- Where were you? Who was there? What did you notice (sounds, smells, feelings)?
- What about the situation was similar to the past, and what was different?
- How are you different than you were in the past?
- What resources, support, and choices do you have now that you didn’t then?
- What helps bring you back to the present?
Prioritize safety and support your life in the present
As you reflect on these questions, keep safety at the center. Focus on recognizing your strengths, building your resources, and supporting the life you’re living now.
Part Two: Dealing With Nightmares
It’s relatively common for people who’ve experienced sexual abuse in childhood to experience nightmares. The challenge of nightmares is that they can be upsetting on their own while also bringing back reminders of abuse you’d rather not revisit. Below, you’ll find some information about why they happen, along with practical ideas that may help when they do.
How Nightmares Can Affect You
- Be vivid reminders and re-experiencing of traumatic events. They may replay events exactly, appear as fragments, or show up symbolically, with distorted or exaggerated representations of the past with accompanying feelings, anxieties, and fears.
- Bring up feelings associated with past abuse, including loneliness, abandonment, distress, vulnerability, fear, sadness, anger, guilt, and shame.
- Cause real physical reactions such as trouble breathing, chest tightness, sweating, shaking, exhaustion, or fatigue.
- Trigger upsetting thoughts and reminders of abuse.
- Disrupt established sleep routines, create fear around going to sleep or sleeping alone or with others, reduce sleep quality, and lead some people to use alcohol or drugs to get through the night.
- Exhaust us, meaning we don’t get the physical and mental health benefits of a good night’s sleep that allow us to function and enjoy the day ahead.
Some of these impacts can persist throughout the day and have long term effects on overall well-being.
Nightmares can be especially hard to manage because they often arrive without warning, can be difficult to understand, and—when linked to abuse—may feel hard to talk about. It’s understandable that men who have experienced abuse may dwell on the content of nightmares, trying to make sense of them.
What Can Help
While nightmares are distressing, there are short-and long-term ways to manage them. Before exploring the content of the nightmares (which can stir things up), it’s helpful to first focus on building a healthy sleep routine.

- When possible, aim for a consistent routine, going to bed and waking up around the same time each day.
- Build a relaxing bedtime routine: stretching, listening to calming music, reading, or doing anything relaxing for 30 minutes before bed. Some people find white noise and sleep apps helpful, too.
- Limit screens or stimulating activities before bed, which can make it harder to fall asleep.
- Make the place you sleep as comfortable as possible.
- Avoid watching the clock, which can increase anxiety and make it harder to fall asleep.
- Get some natural light and/or add slow movement to your morning routine to help regulate your internal clock.
Sleep restores you mentally and physically. With better sleep, it’s easier to cope with difficult symptoms.
If You Wake Up From a Nightmare
- Remind yourself: “I’m safe. This is not happening now.”
- Ground yourself in the present and as the adult you are today (use the grounding resources above and in the StrongAfter Strength Toolkit).
- Breathe slowly and deeply.
- Notice your body’s reactions and remind yourself they are natural responses to trauma. Continue breathing slowly and deeply, and gently imagine your muscles softening.
- Reorient to the present by looking around, turning on lights, touching nearby objects, standing up if possible, looking in the mirror, or speaking to yourself in a reassuring way.
- If it helps, check locks or walk around briefly to reassure your body.
- Drink water, wash your face, or take a shower.
- Refocus your mind: read something light, listen to calming music, do a relaxation exercise.
Tell Someone You Trust
They don’t need to know the details; just sharing that your sleep is disrupted and distressing can help. We all benefit from having someone in our corner who can provide a listening ear and help us access support.
Re-Storying Recurring and Distressing Nightmares
When nightmares keep coming back and become disruptive to your life, some people find it helpful to “re-story” a recurring dream with the following exercise, when you’re feeling safe and supported to do so:

- Choose a recurring nightmare that is not the most intense and not a direct replay of the abuse.
- Write down what occurs in the nightmare (a journal can be good for this), from the beginning, in as much detail as you feel comfortable. You do not need to over-describe upsetting content within the dream.
- Write down the place, what is happening, who is there, and what you’re feeling.
- Then, rewrite the nightmare with a new ending. Note what you’re feeling in this revised version and edit the script so that you feel how you would like to feel at the end of the dream.
*Remember: it’s your choice to do this, and at any time you can also choose to stop writing, close the journal, stop thinking about the dream, and do something else.
- Take time to get to know this new version of the dream, rehearsing the revised dream each night for about five minutes prior to going to sleep.
- After rehearsing, do a breathing or relaxation exercise—one you already know and find calming (see the StrongAfter Strength Toolkit). If you wake during the night, returning to the same exercise can help you settle again.
- When you are satisfied that you have re-storied the nightmare to suit you and it is no longer causing you distress, you might choose to work on another that is slightly more intense than the last (note: it’s not recommended to work on more than one or two nightmares in a week).
This is just one possible approach to dealing with nightmares. If it doesn’t feel helpful, or if it starts to bring up daytime flashbacks, then stop. There are other options out there, and a qualified, trauma-informed healthcare professional can help you explore them.
Dreams Don’t Always “Mean Something”
Nightmares directly linked to past trauma are less common than many people think. Most dreams—and even many nightmares—don’t have a deeper meaning or require action. While they may reflect things you saw, heard, or felt during the day, they can usually be set aside so you can get on with your life.
Consider Professional Support
Because nightmares linked to childhood abuse are connected to real and distressing events, they can sometimes persist, even when you’ve tried re-storying or changing the outcome of the dream.
If nightmares or daytime reminders continue to disturb you, it can be helpful to talk with a qualified, trauma-informed healthcare professional. Relief is possible, and you don’t have to face this on your own.
A Final Encouragement
Acknowledgement: This article was developed with reference to Krakow, Hollifield, et al., “Imagery Rehearsal Therapy for Chronic Nightmares in Sexual Assault Survivors with Posttraumatic Stress Disorder,” Journal of the American Medical Association, Vol. 286, No. 5 (August 1, 2001).
Disclaimer: The information on this page is general in nature and is not a substitute for professional advice. We encourage you to prioritize your safety and well-being and to consider seeking support from a qualified healthcare professional if needed.



